Five years ago today, we said goodbye to our first baby. I was five months pregnant—twenty weeks to be exact—when my doctor told us that the baby was not growing properly and that its head and chest cavity were swollen with fluid. These conditions were, in his words, “not compatible with life.” He told us it was only a matter of time before the heart stopped beating.
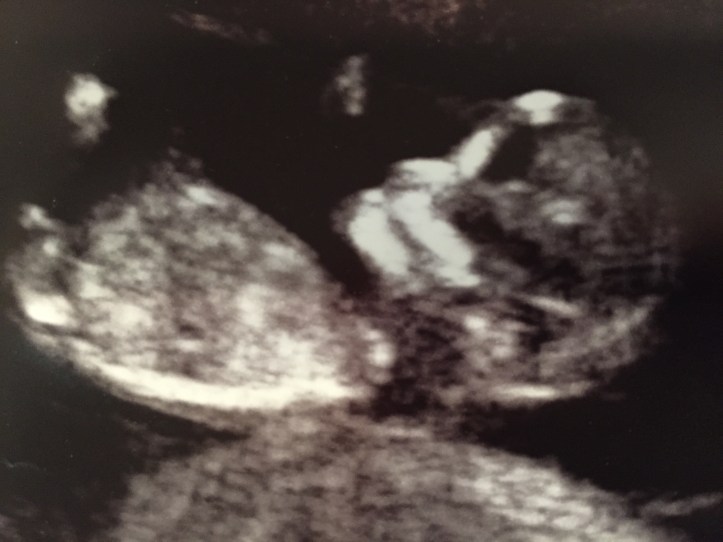
It was the last thing we were expecting to hear. We had gone to the appointment full of excitement—it was time for the anatomy scan, and we were hoping to finally learn the sex of the baby. My mother had started crocheting blankets. I could feel the baby moving. But after the doctor delivered his terrible news, we asked him not to tell us if it was a boy or girl. I couldn’t bear to know.
So I went from daydreaming about nursery themes to preparing for our baby’s death. At that point, we had two options: the doctor could induce labor, or I could have a dilation and evacuation—a late-term abortion. (Staying pregnant and letting nature take its course was not an option. Whatever was causing the swelling in the baby was making my body fill with fluid as well, and continuing with the pregnancy would be too risky.)
I chose the D&E. The “dilation” part of the procedure took a week and involved a series of painful procedures, during which I cried and screamed and then, ridiculously, apologized to the doctor. At the second appointment, before the doctor began, one of the nurses pressed a string of rosary beads into my hand.
And then, at the end of the week, on September 30, 2010, I went to the hospital for the surgery. Afterward, when they wheeled me out to the car, I tried not to look at the other women who were leaving with balloons and bundles in their arms.
Several long, frustrating months followed. For a while, my body behaved as if it had given birth. Thanks to postnatal hormones, my hair fell out in clumps, my breasts leaked milk, and I got so sweaty at night that I had to sleep on towels.
The doctors still didn’t know what had gone wrong, and they cautioned us against trying to get pregnant again until they had figured it out. They believed it was some kind of genetic abnormality, but beyond that they were pretty clueless. So Steven and I became investigators. We relearned everything we’d forgotten about genes and chromosomes and Punnett squares. We reached out to doctors and geneticists and submitted to all kinds of blood tests. Our detective work helped to distract me from the grinding monotony of my grief.
In the meantime, other babies continued to be born. My brother and his wife had a boy, and my best friend gave birth to a girl. I lived in Brooklyn at the time, and it seemed to me that the entire female population of the borough was either pregnant or had a baby in tow. My due date, February 8, came and went.
Finally, our medical mystery was solved. We learned that Steven and I are both carriers of thalassemia, a blood disorder that disrupts the production of hemoglobin. In its mildest form, it’s virtually symptomless; at its most extreme, it’s fatal. The baby had had the most severe form of alpha thalassemia, which meant that its body could not produce hemoglobin at all. Most babies with this condition are stillborn or die soon after birth.
Along with this information came the answer to the question we hadn’t dared ask back at the doctor’s office in September. I was going through the thick packet of medical records I’d requested from the doctor when I saw it: the baby had been a girl.
The word thalassemia is Greek for “sea blood.” It got its name because the first cases were identified among immigrants who had come to the United States from regions along the Mediterranean Sea (mostly Greeks and Italians, like Steven and me). It has a romantic ring to it, like sailors yearning for an adventure. But for our daughter it was a cruelly literal description. Her body, unable to produce blood, had filled itself with water instead.
We could have tried getting pregnant again the old-fashioned way, but doing so would have meant facing a one-in-four chance of losing another baby. So we decided to go the science route. That meant first doing a course of IVF at NYU Fertility Center. The idea was to end up with a few embryos that could then be screened for thalassemia. This is called pre-implantation genetic diagnosis, or PGD.
The geneticists who would do the screening were based out in California at a place called Gene Security Network—a name that made me envision a secret bunker located deep underground. Apparently, a test did not yet exist for the type of thalassemia we have, so they would have to create the test first. They weren’t sure they could do it. If they managed it, they would use that test to determine which embryos were thalassemia-free, and then the NYU doctors would transfer one of the healthy embryos into my uterus, where, hopefully, it would decide to take root.
Amazingly, it all worked according to plan.
I started my first IVF cycle in the spring of 2011. That cycle yielded twenty-six eggs, which, when coupled with Steven’s sperm, resulted in seventeen embryos. Ten of those were deemed good enough to biopsy for genetic testing, so the embryologists at NYU took a few cells from each and sent them off to Gene Security Network.
Romantic, right?
In the end, we got four healthy embryos—which, for anyone undergoing IVF, is an embarrassment of riches. And, in a bittersweet twist, all four of them turned out to be boys.
The first embryo was transferred in July 2011, and in March of the following year, Theo was born. We decided to try for number 2 in October of 2013. Sadly, that one didn’t take. We gave it another shot in March, traveling into Manhattan from our home in New Jersey on St. Patrick’s Day. That embryo became Nicholas, who was born last November.
One embryo remains.
For various reasons, we have decided that our family is complete. So we found ourselves facing another decision: We could have the remaining embryo disposed of as medical waste; we could allow NYU to use the embryo for research; we could donate the embryo to another family who is unable to have a baby on their own; or we could have the embryo transferred into my uterus at a time when it is impossible for me to become pregnant, thereby letting my body dispose of it naturally.
It was pretty much a no-brainer to donate the embryo for research. If the embryologists can learn something that enables them to help more people have families, then what more could you ask for? I knew that I wouldn’t be able to give it to another family, as wonderful a gesture as that would be; I would go insane thinking about one of “my” children out there somewhere in the world. Nor could I allow it to simply be thrown away. And having it transferred with no chance of conception just seems… pointless.
And yet. I am finding it incredibly hard to make it final. We have now gotten three letters in the mail warning us that we owe $1,000 for the embryo’s annual storage fee. (A steal for Manhattan rent, but still.) We are out of time. We either have to send a check or sign the research waiver.
This whole process, from the baby we lost to the embryo that remains, has made me ask myself some hard questions. It has challenged notions that I had previously taken for granted—about abortion, about when life begins. It also has shown me how very lucky we are.
We are lucky to live in a time in which science and medicine make it possible for people with fertility and medical issues to have healthy children—and we are extremely fortunate to be able to afford to take advantage of it. We are lucky to live in a state in which late-term abortions are an option. Many others are not so lucky. Some must travel elsewhere—if they can afford to do so. If they can’t, they have no choice but to endure suffering that could have been avoided.
Last week, when I was on a walk with my dog, I passed a woman sitting on a bench with her infant daughter. Seeing little girls often makes me think of the one I lost, but this time it really got to me. I started to tear up and was soon choking back sobs. I was a wreck. After a few minutes of this, it occurred to me: the date was September 23, exactly five years to the day since the doctor’s appointment when we learned that the baby wouldn’t survive. I had never kept that date in my head; I’d only remembered the 30th, which is when I went into the hospital to have the surgery (I still find it difficult to call it an abortion). When I got home, I looked through old e-mails to double-check, and I was right.
I don’t usually buy into these woo-woo, touched-by-an-angel moments, but I have to believe in this one.
I also have to believe that this last embryo will help advance the science that allowed us to have our two healthy, amazing (and incredibly handsome) boys. Because, having thought it through over and over, I can say with conviction that this embryo is simply a bunch of cells. It is not a baby. And, just like the first one, it was not meant to be ours. But it is still so hard to say goodbye.

I am so sorry that you lost your baby girl…I lost my daughter at almost 24 weeks
LikeLike
Thank you so much. I’m sorry for your loss, too. xo
LikeLike
So much of what you wrote could’ve been taken from my own experience. It’s been 15 months and life is back to normal and yet, it is always with me. It was blow after blow of cruelties; from learning the news that “the situation will not sustain life”, learning firsthand that anyone who thinks “late term abortions” are an easy choice should never utter words again because the emotional and physical pain is more than any human should experience and the betrayal I felt from my own body in the post pregnancy symptoms that lasted for months. My failed pregnancy lead to underlying medical issues coming to light so in some ways, my baby helped save my life even though he couldn’t stay with us. Thank you so sharing your story, you are so brave and it’s appreciated.
LikeLike
Alex, thank you for writing. I’m so sorry for what you had to go through. Be well and good luck to you. xo
LikeLike
You are an amazing mom and woman. Thank you for sharing your beautiful heartfelt story of life 💜
LikeLike
[…] also written other things about my experience with pregnancy loss here on the blog and for a site called Mothers Always […]
LikeLike